If you’ve been dealing with IBS for a while, there’s a strong chance you’ve already downloaded at least one app. As a health researcher and Master’s nursing student, I often come across people who are trying, often desperately, to make sense of symptoms that don’t behave consistently.
IBS is generally understood as a disorder of gut-brain interaction, where gut function, sensitivity, and nervous system signaling all overlap. In reality, though, it rarely follows a clear pattern because symptoms can shift over time. For example, you might experience constipation one week and urgency the next. Foods that felt okay last month can trigger new, disruptive symptoms the next. Stress, sleep, travel, and routine changes all play a role, sometimes in ways that are hard to pin down.
If you search for the best apps for IBS, you’ll find plenty of options promising explanations. Although many of these apps are genuinely useful, there’s an important difference between tracking symptoms and having a more joined-up plan in place.
Topic Contents
The Types of IBS Apps that are Available
Most IBS apps focus on only one part of the picture.
Some are built around food. The Monash FODMAP app, for example, is widely used to help people navigate elimination and reintroduction. It brings structure to what can otherwise feel like a long list of “maybe avoid this” advice, which can become overwhelming quite quickly.
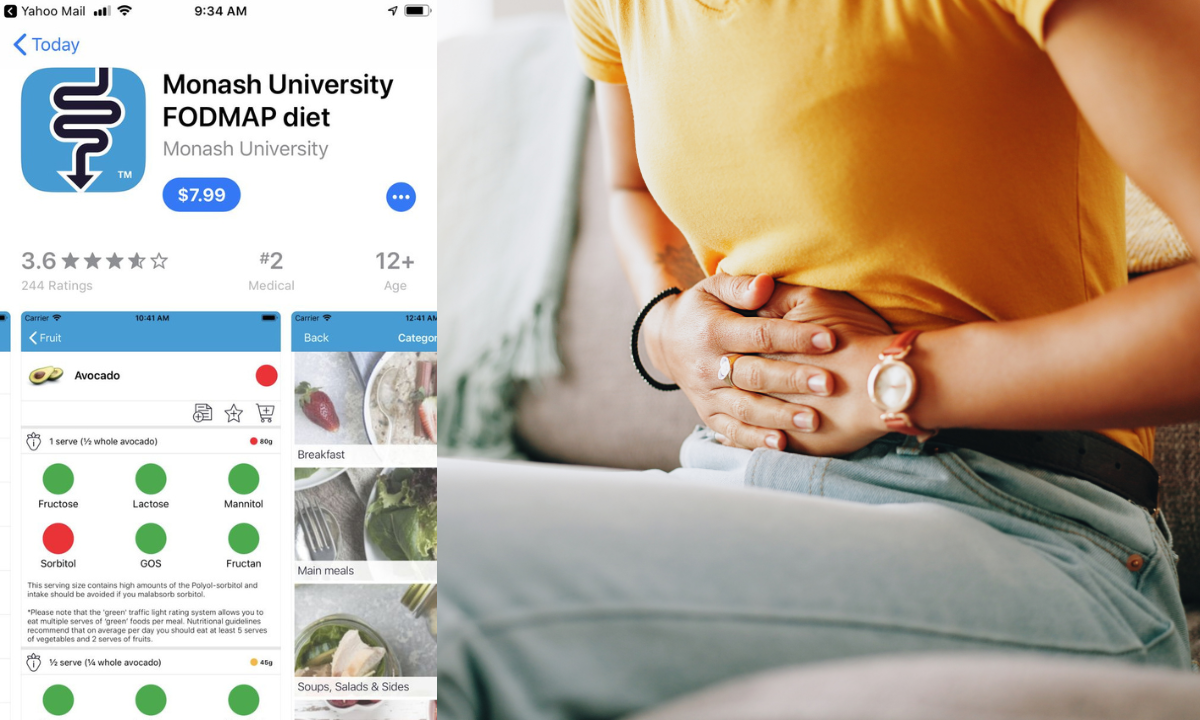
Others focus on tracking. Apps like Bowelle let you log symptoms, meals, bowel habits, and daily patterns, often alongside things like stress, sleep, or energy levels. Over time, that kind of tracking can make patterns easier to spot, especially ones that aren’t obvious day to day.
It also means you have something concrete to refer back to. That can be helpful when you’re trying to explain symptoms, or when you eventually speak to a clinician and need to piece together what’s been happening over time.
Then there are gut-brain tools. Nerva is one example, built around a structured program of gut-directed hypnotherapy. The aim is not to change the gut directly. Instead, it focuses on how the brain processes gut signals. This can reduce sensitivity and help symptoms feel more manageable over time. For people whose symptoms clearly flare with stress or anticipation, this kind of approach can be a useful addition.
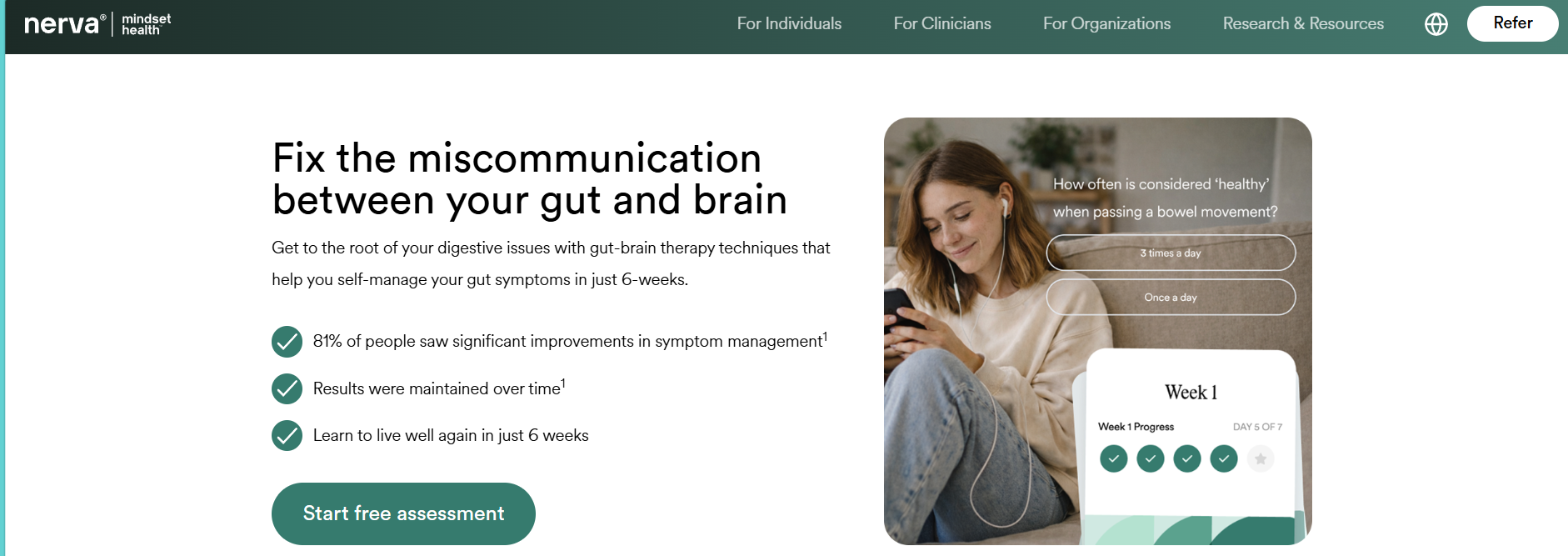
Taken together, these tools point to something important; that IBS does not have a single cause. It tends to sit across several systems at once, and most apps are designed to support one part of that at a time.
Where IBS Apps Can Help
For many people, apps are a useful starting point since they make symptoms feel more tangible. Instead of trying to remember how you felt three days ago, you have something concrete to look at. That reassurance alone can make a difference.
Tracking may help you notice patterns like particular foods and timing, and sometimes those patterns are enough to guide small changes that could improve things. It also comes up a lot that people can feel more prepared when they eventually speak to a clinician. Having a record, even a rough one, makes it easier to explain what’s been going on. In some cases, that is enough to move things forward. But this is also where things can start to stall.
At a certain point, however, more tracking does not necessarily lead to more clarity.
You might have weeks or months of data but still feel unsure what it means or how to move forward. Or maybe you identify patterns, make changes, and nothing improves in a meaningful way. Sometimes symptoms will improve briefly, then come back in a slightly different form.
Most apps are good at collecting information or delivering one specific type of support. What they do not always do is bring that information together into a clinical plan that can be adjusted over time. The result is often a lot of data, but no clear direction.
If you’ve tracked everything and nothing has really changed, or you’re trying several approaches at once, adjusting diet, using stress tools, and changing routines, it may be time to rethink the plan.
As symptoms change, which they often do with IBS, knowing what to do next is no one-size-fits-all.
How Different IBS Care Options Fit Together
If you look at the landscape of care for IBS, most support falls into a few categories. In my experience, a multifaceted approach to IBS is advisable: some form of medical input, dietary guidance that is more structured than trial and error, and support for the gut-brain side of symptoms, especially when stress or anticipation plays a role.
Follow-up is a big part of this, and it is often the piece that is missing. Symptoms shift over time, and what works for a few weeks does not always hold.
The challenge is that the different dimensions of IBS care are often accessed separately. You might see a clinician for one symptom, a dietitian for another, and try an app for something else, but they do not always converge in a meaningful way.
Apps and digital tools can help with tracking, education, or specific approaches like gut-directed hypnotherapy. They are often the first step, and for some people, they are enough to get started.
General telehealth platforms, like Teladoc or Amazon One Medical, tend to be useful when you need to speak to someone quickly, whether that is for initial advice or short-term support. They are built for broad care rather than ongoing IBS management.
Dietitian services can be particularly helpful if food feels like a major driver. They bring structure to dietary changes, which can otherwise feel quite open-ended. But they do not typically cover medical assessment or the gut-brain side of symptoms.
Traditional gastroenterology care plays an essential role, especially for diagnosis and when testing or procedures are needed. In practice, though, follow-up around diet or behavioral support often sits in separate pathways, which can take time to access.
Each of these approaches can help in the right context, but most people end up moving between them rather than having them work together.
Where a Coordinated Approach Can Come in
For people whose symptoms keep cycling despite trying different approaches, the missing piece is often coordination.
This is where models like Oshi Health enter the equation. Oshi Health is a virtual, evidence-based gastroenterology clinic focused on digestive conditions like IBS. Care is structured as a program rather than a series of disconnected visits. Patients typically work with a small, dedicated team, including a GI provider with advanced training, a registered dietitian, and a behavioral health provider focused on gut-brain support, with oversight from board-certified gastroenterologists.
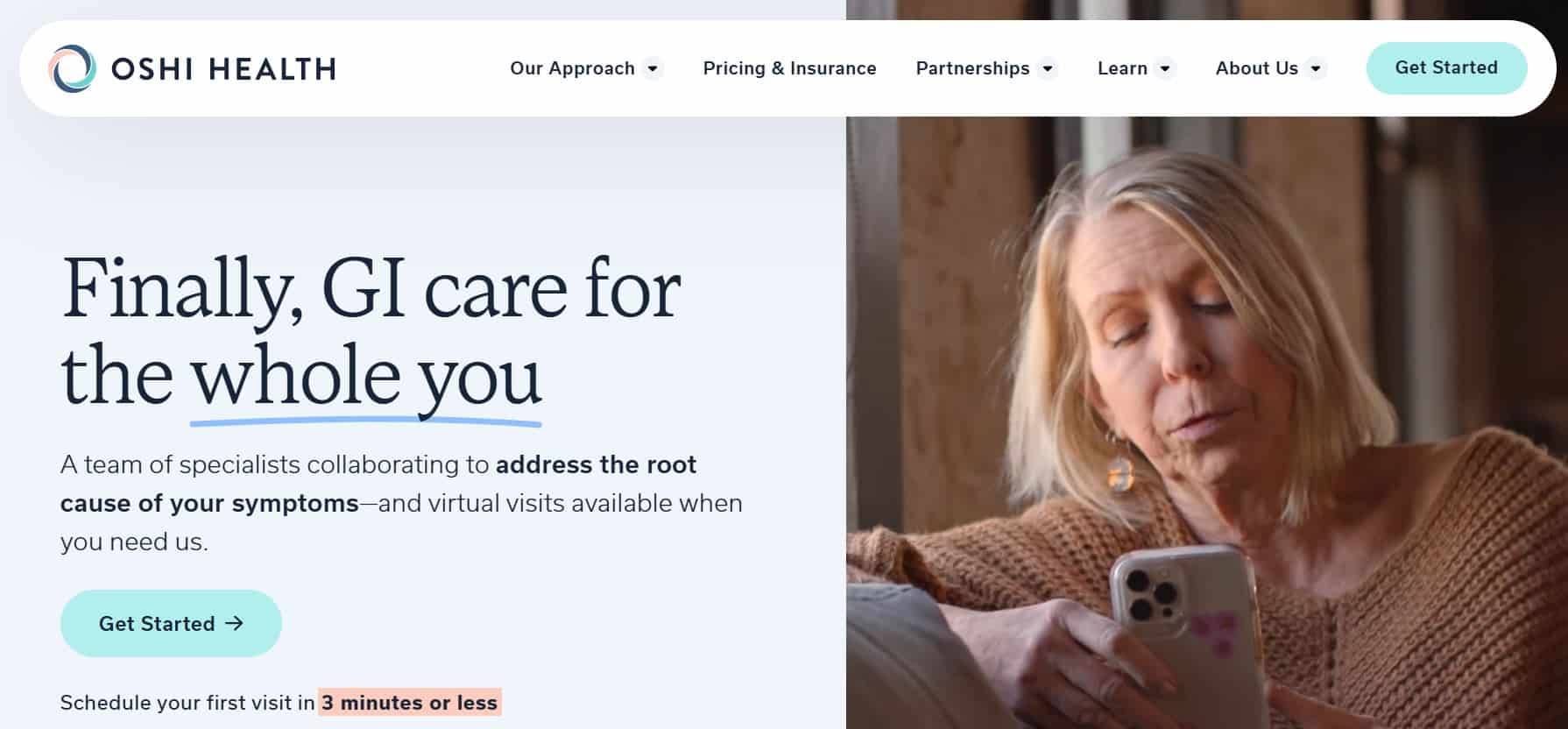
Care usually starts with a detailed virtual assessment, closely reviewing symptom patterns, history, and any previous testing. From there, the plan may include medication, dietary strategies, and gut-brain support, adjusted over time as symptoms change.
Instead of trying to manage each piece separately, care is brought together and revisited as needed. Access is also part of the picture. Oshi works with many major insurance plans, and appointments are typically available within days rather than months. Oshi Health is also available via an app, giving patients the option of a more digital-first experience if they prefer. As with any care, individual results vary, but the model is built around ongoing support rather than one-off input.
How to Decide What Makes Sense for you
Where you are in your journey with IBS will inform what will help most.
If you are early on in trying to understand what is happening, apps can be a good place to start. They help build awareness and give you something to work from. If you need quick support, especially during a flare, general telehealth can be a practical option.
If food patterns are clearly driving symptoms, working with a dietitian may add useful structure. However, if symptoms are ongoing, unpredictable, or not responding to these steps, it is often a sign that you need something more integrated. A plan that looks at medical, dietary, and gut-brain factors together, with enough follow-up to adjust along the way.
IBS apps can help you track what is happening and offer a sense of control when things feel unpredictable. But they only provide one piece of the puzzle. The difficulty isn’t spotting patterns, but instead knowing how to respond to them in a way that actually holds up over time.
That is where more coordinated, GI-focused care can make a difference. Not by replacing the tools you have already tried, but by building on them with a plan that evolves as your symptoms do.
Danielle (Dani) Mathieu is a health and medical writer who works with global health and wellbeing businesses to deliver insight-driven, research-backed content at the intersection of psychology and nursing. She has 18+ years of experience in communications, holds an MA in Psychology, and is currently studying for an MSc in Adult Nursing.
Dani is happiest when she’s translating complex health and nutrition science into plain-English stories that feel genuinely useful without being overwhelming. When she’s not juggling clinical placements on the ward, she’s usually writing. She lives on the Scottish coast, loves a cold sea breeze, and is often accompanied by a very opinionated dog.







