Living with irritable bowel syndrome is rarely simple.
For some people, IBS can show up as unpredictable abdominal pain and severe bloating that makes it difficult to get through a normal workday. For others, it’s a constant calculation of where the nearest bathroom is. Meals can become experiments, and travel requires scrupulous planning.
What makes IBS extra frustrating is that symptoms can be inconsistent. One week, it might be constipation and discomfort after eating. The next week it’s diarrhea. Stress, sleep, diet, and routine can all shift the picture, and even when medication helps, it often doesn’t solve everything.
As a health writer and researcher currently completing an MSc in Nursing, I’ve dedicated time to looking at how clinicians approach IBS and how people experience it on a day-to-day basis. Although many people eventually receive a diagnosis, what tends to follow is a longer stretch of trial and error: diet changes, medication adjustments, and advice that works for a while and then stops working. This middle phase, where symptoms keep cycling, but care can be fragmented, is one reason why online IBS programs have started gaining more attention.
Topic Contents
Why IBS Care Is Often Incomplete

Traditional gastroenterology care plays a central role in diagnosing digestive conditions and ruling out more serious disease. Many people first encounter IBS within that system, yet, the difficulty often comes after.
IBS does not show typically up on imaging scans or routine blood tests. Diagnosis also usually relies on symptom patterns and clinical criteria once other conditions have been excluded. From a clinical standpoint, this approach is well established, but from a patient perspective, it can feel less definitive.
Many people leave their appointment with medication or a list of dietary suggestions. Sometimes symptoms improve, sometimes they settle briefly and then return months later.
Part of the challenge is time; gastroenterology appointments can often be limited, and follow-up visits may be spaced months apart. Simultaneously, access to registered dietitians is inconsistent across insurance plans. Behavioral or gut-brain support, which research increasingly links to IBS symptom patterns, may sit in an entirely separate referral pathway.
The result can mean patients receive fragmented care. Often, patients will then end up trying to connect these pieces on their own.
When IBS Is Suitable For Online Care

Not every digestive condition should be managed remotely. Some symptoms require prompt in-person evaluation. However, IBS is one of the gastrointestinal conditions that can often be managed effectively through telehealth once serious conditions have been ruled out.
IBS diagnosis and treatment rely heavily on symptom history, trigger patterns, and how symptoms respond to treatment over time rather than a single diagnostic test. Clinicians usually look closely at patterns across daily life, considering symptom history, bowel habits, possible dietary triggers, and whether factors like stress, sleep, or medication changes appear to influence flare-ups.
These conversations can work really well in virtual care settings where follow-up is easier and symptom patterns can be reviewed over time. Telehealth also allows clinicians to adjust dietary approaches gradually, review symptom tracking, and check in when flare patterns change.
There are still situations where in-person care is important. Symptoms like blood in the stool, black or tarry stools, unexplained weight loss, persistent vomiting, iron-deficiency anemia, severe abdominal pain, or new gastrointestinal symptoms beginning after age 50 should always prompt direct medical evaluation.
Excepting these, for people living with established IBS symptoms, virtual care can offer a practical way to manage the condition over time.
What a Good Online IBS Program Will Offer

One of the most common misconceptions about IBS care is that it can be resolved through a single intervention.
IBS is considered a disorder of gut-brain interaction. This means symptoms are influenced by several overlapping factors, including gut motility, visceral sensitivity, diet, and nervous system signaling between the digestive system and the brain. That complexity explains why IBS rarely improves with just one change.
Treatment can, in turn, look multifaceted: medication may help regulate bowel patterns or reduce abdominal pain, while dietary strategies can help identify triggers that worsen symptoms. Stress management approaches can, in turn, calm the feedback loop between the brain and the gut that often amplifies flare-ups. And sleep patterns, daily routine, and lifestyle factors can also play a role.
There are also different formats for care. Strong IBS care programs will usually address several of these elements together rather than treating them as separate issues (this is one of the key differences between basic telehealth visits and more structured IBS care programs). Some telehealth platforms, meanwhile, offer single appointments where a clinician can provide short-term guidance or prescribe medication. During an acute flare, this can be particularly useful.
Best Overall Online IBS Program: Oshi Health
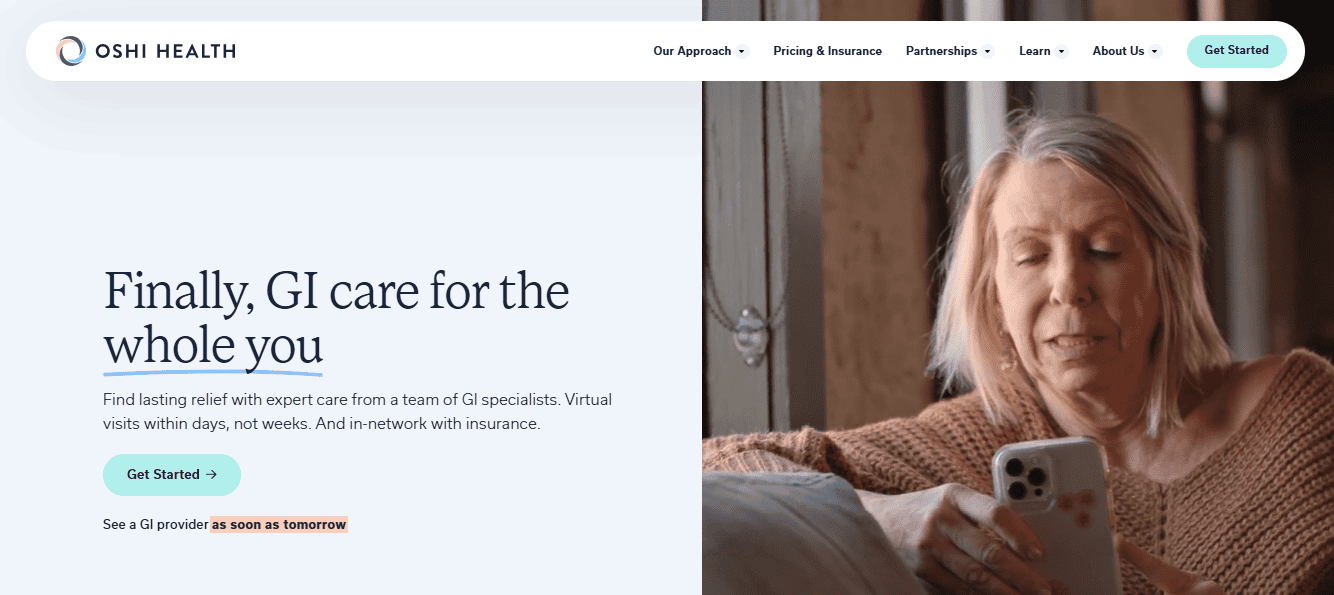
One example of this type of coordinated care is Oshi Health, a virtual clinic focused entirely on digestive conditions. Oshi operates as a virtual gastroenterology clinic designed to treat conditions such as IBS, acid reflux, inflammatory bowel disease, and persistent digestive symptoms.
Care is delivered by a multidisciplinary team, starting with a GI provider (nurse practitioner or physician assistant) with specialized training in digestive health. Patients may also work with a registered dietitian and a gut-brain specialist. All care is guided by board-certified gastroenterologists, who provide oversight and medical guidance, though patients typically meet directly with their GI provider and specialists. Medication alone will likely not resolve the condition. Diet, stress responses, nervous system signaling, and bowel motility all influence how symptoms develop and fluctuate. Addressing these elements together allows treatment plans to evolve as symptoms change.
Oshi organizes care as a structured program rather than a series of disconnected appointments. Patients usually begin with a detailed virtual consultation reviewing their symptom history, previous testing, and treatment experiences.
From there, the care team develops a personalized plan that may include medication adjustments, dietary guidance, and gut-brain strategies. Follow-up appointments allow the plan to adapt over time as symptoms change.
Because the clinic operates virtually, appointment availability may also be faster than traditional referral pathways. Oshi works with many major insurance plans, so it’s affordable for many patients.
According to reported outcomes published by Oshi, many patients are able to schedule their first visit within about ten days. Oshi also reports that:
• 92% of patients experienced symptom relief within 10 weeks
• 88% of previously undiagnosed patients received a clear diagnosis within three months
• 98% of patients report satisfaction with care
For patients who have already tried basic IBS treatments without lasting relief, this type of coordinated care model closely reflects current clinical guidance for managing disorders of gut-brain interaction.
Other Online IBS Pathways
Oshi is not the only option people researching IBS care will encounter. The broader telehealth landscape includes several different types of services that address different parts of the IBS experience.
Understanding what each type provides can help set realistic expectations.
General Telehealth Platforms
Large telehealth providers such as: One Medical, Teladoc, Doctor on Demand, and Amwell offer convenient access to primary care clinicians.
These services can be useful for initial symptom evaluation, medication refills, or short-term support during flare periods. In some cases, they may also refer patients to gastroenterology specialists when symptoms require more focused care.
However, these platforms are designed primarily for general medical care rather than ongoing IBS management. Long-term digestive care often requires additional specialist input.
Digital Gut–Brain Tools
Some digital programs focus specifically on the behavioral side of IBS symptoms. One example is Nerva, a mobile program based on gut-directed hypnotherapy.
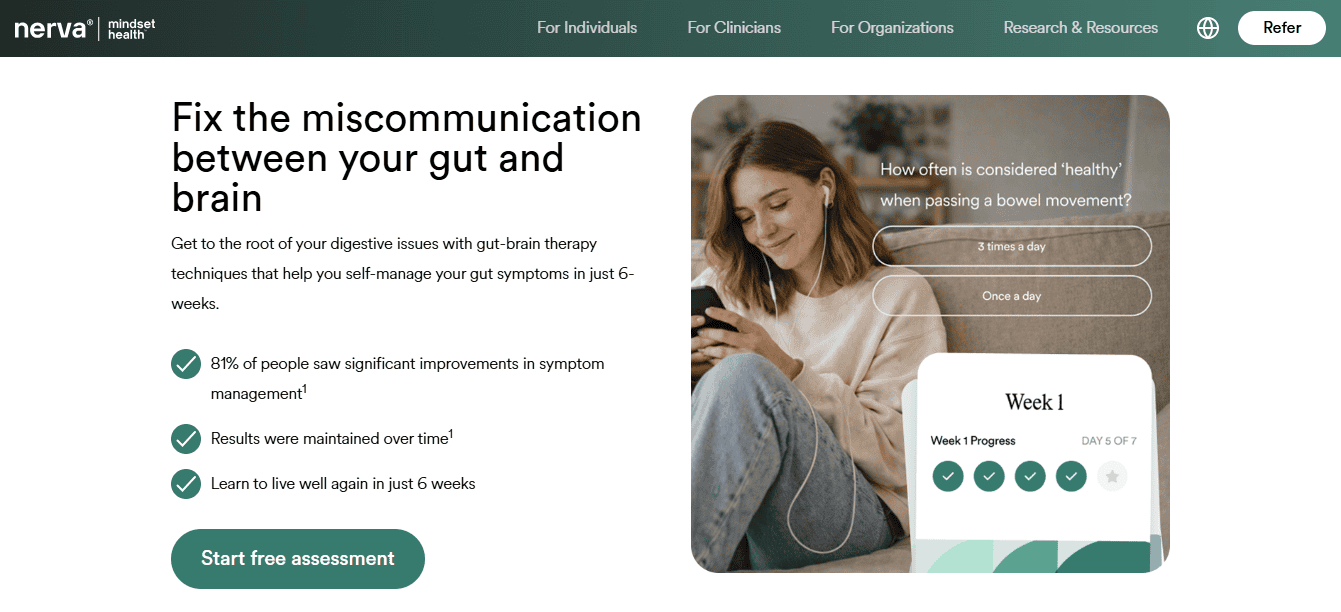
Nerva delivers guided audio sessions designed to calm the gut-brain communication pathways involved in IBS symptoms. Some patients find these approaches helpful, particularly when stress and symptom anticipation appear to worsen flare patterns.
These tools do not provide diagnosis, prescription management, or medical testing coordination. They are often used alongside clinician-led care rather than as standalone treatment.
Microbiome Testing Platforms
Another category people often encounter during IBS research involves microbiome testing.
Companies such as Viome offer stool tests designed to analyze gut microbiome patterns and generate personalized dietary suggestions.
These services can provide interesting insights about gut bacteria, but they are not clinical care programs. Results are typically delivered through digital reports rather than consultations with gastrointestinal specialists. For people seeking structured IBS management, microbiome testing is generally considered informational rather than diagnostic care.
Functional Medicine Memberships
Some patients prefer a broader lifestyle-focused approach to chronic health conditions.
Programs such as Parsley Health operate using a functional medicine model that emphasizes longer appointments and an investigative approach to symptoms. Such programs often include extensive testing and membership-style care, however, insurance coverage varies depending on the provider and plan.
Whilst many patients value the time and lifestyle focus these models offer, others prefer gastrointestinal care programs that follow more traditional GI treatment pathways.
Dietitian Networks
Telehealth dietitian platforms have also become more widely available. Examples include Nourish and Berry Street.

These more focused networks connect patients with registered dietitians who can help identify dietary triggers and guide approaches such as low-FODMAP diets. Dietary guidance can be very helpful for IBS management. However, dietitian-only services typically do not include medical evaluation, prescription management, or diagnostic testing. For many patients, diet support works best alongside medical care rather than instead of it.
When Online Care Is Not Enough

Virtual care can be extremely helpful for managing IBS symptoms, but it is important to recognize when in-person care is needed, as certain symptoms should always be evaluated in-person. These include blood in the stool, severe or sudden abdominal pain, persistent vomiting, unexplained weight loss, or signs of dehydration.
People living with inflammatory bowel disease or other diagnosed digestive conditions may also need periodic in-person testing, such as imaging, colonoscopy, or laboratory work.
In many cases, virtual GI programs work alongside traditional care rather than replacing it. A telehealth provider can help manage symptoms, adjust treatment plans, and coordinate referrals when additional testing is necessary.
This hybrid model is becoming increasingly common. Patients receive ongoing support virtually while still accessing in-person diagnostics when required.
Key Takeaways
Choosing an online IBS program depends on several factors. Symptom severity, insurance coverage, and access to specialists all play a role. General telehealth platforms can provide quick medical advice or help during flare periods. Dietitian services can offer useful nutritional guidance. Digital gut-brain tools may help reduce symptom sensitivity for some people. However, individuals dealing with persistent IBS symptoms often benefit most from programs that combine gastrointestinal medical care, dietary guidance, gut-brain support, and ongoing follow-up.
That is where Oshi Health stands out as one of the strongest overall options in the current telehealth landscape. Its model reflects something clinicians increasingly recognize. IBS rarely responds to a single solution. Effective care looks at the full picture. How the gut behaves. How the brain responds. How everyday life influences both.
For many patients, having a coordinated care team that understands those connections will make IBS feel less like an endless cycle of symptoms and more like a condition that can actually be managed.
Danielle (Dani) Mathieu is a health and medical writer who works with global health and wellbeing businesses to deliver insight-driven, research-backed content at the intersection of psychology and nursing. She has 18+ years of experience in communications, holds an MA in Psychology, and is currently studying for an MSc in Adult Nursing.
Dani is happiest when she’s translating complex health and nutrition science into plain-English stories that feel genuinely useful without being overwhelming. When she’s not juggling clinical placements on the ward, she’s usually writing. She lives on the Scottish coast, loves a cold sea breeze, and is often accompanied by a very opinionated dog.







