If you’ve ever used sleeping pills to help you fall asleep, you may have noticed that over time, the quality of your sleep can start to feel off.
Maybe you still fall asleep, but wake up feeling groggy, or your sleep just doesn’t feel as restorative as it once did. In my own experience, I’ve found that many people begin to look for alternatives when they realize sleeping pills aren’t offering the full, restful sleep they need.
While medication can be helpful for short-term insomnia, it’s really just addressing one part of the sleep process: getting you to sleep faster. But better sleep is about finding a deeper, restorative rest and balancing all the systems that keep you sleeping soundly through the night.
That’s where sleep devices come in. They’re often marketed as “alternatives to sleeping pills,” but they actually work differently, targeting specific barriers to better sleep. I’ve seen firsthand how these devices can support a more natural sleep cycle, whether it’s stabilizing your sleep environment, calming your nervous system, or helping your brain transition into deeper sleep states.
If you’re looking to improve your sleep, it’s important to choose a device that fits your specific sleep struggles. For people with chronic insomnia, the most evidence-supported first-line treatment remains Cognitive Behavioral Therapy for Insomnia (CBT-I). Guidelines from the American Academy of Sleep Medicine recommend behavioral and psychological approaches as a primary treatment, particularly when sleep difficulties are ongoing.
Topic Contents
When and When Not to Use Sleep Devices

There are times when devices may not be the right starting point. For example, if you experience loud snoring, choking, gasping, significant daytime sleepiness, or unusual nighttime behaviors, these could be signs of an underlying sleep disorder that needs medical attention.
With that in mind, when devices are appropriate, they can be a great way to support better sleep. However, it’s important to recognize that these devices don’t all work in the same way. They often get lumped together as “alternatives to sleeping pills,” but they target different aspects of the sleep process, which is why switching between devices without understanding how they work might not lead to meaningful results.
To make sure you’re addressing the right issue, it’s helpful to break down sleep devices into three main categories:
- Tools that stabilize your sleep environment and routine
- Tools that help calm the nervous system
- Tools that support your brain’s transition into sleep
Each of these categories tackles a different barrier to better sleep. The key is matching the tool with the root cause of your sleep issue. In my experience, many people struggle with multiple devices because they’re not addressing the right problem.
To get started, think about what’s actually keeping you from a good night’s sleep: Is it your environment, your level of alertness, or difficulty getting your brain to transition into deeper sleep? The body’s systems, like circadian timing, nervous system balance, and brain activity, all work together to maintain healthy sleep.
This is where alternatives like sleep devices can help: by supporting the systems that regulate sleep, they focus on creating the right conditions for natural, restorative rest.
1. Tools for Stabilizing Your Sleep Environment

If you’re dealing with sleep disruptions due to things like noise, inconsistent routines, or even the changing seasons, tools that stabilize your sleep environment can be a good first step. These are typically low-effort, easy-to-use options that tap into well-established sleep science. They may not solve all your issues, but they can make a noticeable difference when used consistently.
Sound machines and sunrise alarms are popular choices. For people who live in noisy areas, or just tend to wake up at every little sound, these tools can work wonders. In many cases, it’s not the loudness of the sound that wakes you, it’s sudden change. A consistent background noise can mask those disruptions and help you stay asleep longer.
For others, silence can actually feel unsettling, especially at night. A steady sound, like white noise or calming nature sounds, can create a sense of predictability, helping your brain relax and stay asleep without those little disturbances that make falling back asleep hard.
Light therapy is particularly good for people struggling with circadian rhythm disruptions (which is more common than you might think). Light exposure, especially in the morning, helps reset your body’s natural sleep-wake cycle. If you’ve been waking up too late or feel off during the day, even small adjustments to your light exposure can gradually help get your timing back on track, especially in winter months or if you’re spending most of your time indoors.
When These Tools Fall Short
Where sound machines, light therapy, and similar devices fall short is when the issue lies within your body itself. Many people who struggle to sleep aren’t waking up due to noise or light; they’re waking up because they can’t relax their bodies or calm their minds. In other words, they’re dealing with internal issues like tension, overactive thoughts, or high alertness.
If your problem is internal (like physical tension or an overactive mind) adjusting your environment might help, but it won’t necessarily solve the core issue. This is why you might find that sound machines or light therapy help a bit, but don’t fully resolve your sleep challenges.
Who This Works Best For
These environment-stabilizing tools are most effective for people whose sleep is disrupted by external factors, like noise, light inconsistency, or even environmental changes (such as winter months or daylight savings). They can also work for people who have a lot of interruptions in their sleep schedule.
2. Devices That Calm the Nervous System

If your nights are filled with stress, tension, or a body that doesn’t fully settle at night, devices that focus on the nervous system may help your body move into a more settled state.
These devices, particularly those focused on vagus nerve stimulation, are designed to help shift your body from a heightened “fight or flight” state into a more relaxed “rest and digest” state, making it easier to move toward a sleep-ready state.
There is a growing body of evidence supporting vagus nerve stimulation in areas such as anxiety and emotional regulation. It plays a role in regulating many of the body’s automatic functions, like heart rate, breathing, and digestion.
When the vagus nerve is gently stimulated (often through the skin or ear), it can help slow down your heart rate, reduce muscle tension, and ease the body out of a heightened stress response. The effect is usually subtle, but over time people often describe feeling less physically alert, more grounded, and better able to wind down.
Who This Works Best For
These approaches support the body’s ability to settle, but they don’t directly influence the brain processes involved in falling asleep. For some people, that distinction becomes important. This is why some people find these devices helpful for relaxing, but not sufficient when the main difficulty is falling asleep.
If you feel physically relaxed but still struggle to fall asleep (especially if the issue seems to be timing or brain activity), this type of device may be less effective. In that case, it may be worth exploring approaches that more directly support the brain’s transition into sleep.
3. Neurostimulation Devices: Supporting the Brain’s Transition to Sleep
If you’ve already worked on your environment, your routine, and even stress levels, but still find yourself lying awake, the issue may be in how your brain is transitioning into sleep.
Falling asleep isn’t just about feeling tired. It requires a shift in brain activity from faster, alert patterns to slower rhythms associated with early sleep. For some people, that shift doesn’t happen easily, even when everything else is in place.
This is where neurostimulation devices come in. Instead of focusing on the down-stream nervous system or environment, they aim to support the brain directly during that transition.
One approach used in newer consumer devices is transcranial alternating current stimulation (tACS). This involves delivering a safe, very low-level electrical current through the scalp to gently interact with brainwave activity as you’re trying to fall asleep. The goal is to help guide the brain into those slower, sleep-ready patterns.
Research in this area is still evolving, but early findings suggest it may help some people fall asleep more efficiently or improve certain aspects of sleep quality over time.
Who This Works Best For
It’s important to set expectations here. This is not a quick fix or a one-night solution like medication can be. These devices tend to work more gradually and require consistent use to see results.
This type of approach is usually considered by people who feel they have already addressed sleep hygiene, routine, and stress, but still struggle to fall asleep. It is less about creating relaxation and more about supporting the brain’s ability to transition into sleep.
Somnee: An Example of Neurostimulation in Action

Somnee combines transcranial alternating current stimulation (tACS) with EEG-based sensing, which allows the device to monitor pre-sleep brain activity and adjust stimulation accordingly. This closed-loop approach means the system responds to the individual rather than delivering the same input each night.
In practice, this begins with a short session at the start of the night, typically around 15 minutes. Over time, the system builds a picture of how the brain approaches sleep and adjusts the stimulation based on that.
The process is structured in stages:
- An initial mapping phase
- A personalization phase
- An ongoing adaptive phase
This aligns with the company’s staged model:
- Mapping (sessions 1–7)
- Personalization (sessions 8–21)
- Adaptation (ongoing use)
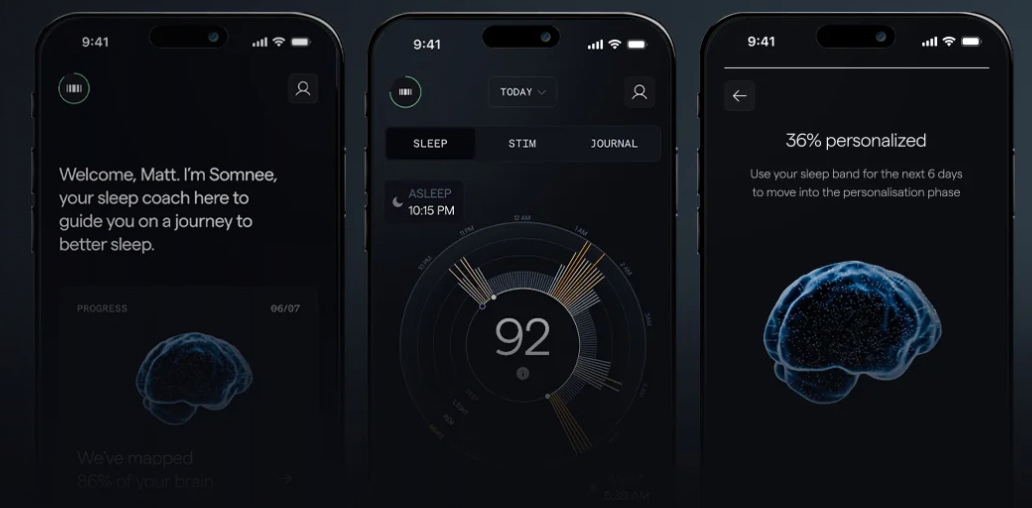
Rather than acting as a one-night fix, the system gradually learns your sleep patterns and adjusts the stimulation over time. After that initial phase, most people shift into a maintenance rhythm, using it every few nights to help reinforce more consistent sleep.
It also includes a feature for middle-of-the-night wakeups, which lets you ease back to sleep without turning on lights or reaching for your phone, something that can easily make it harder to fall back asleep.
From a research standpoint, it’s worth noting that this is one of the few categories in consumer sleep tech with published clinical data behind it. That’s not always the case in this space, where many products rely more on general wellness claims.
In real-world use, this type of approach tends to appeal to people who feel like they’ve already handled the obvious factors but still can’t fully switch off at night, especially those who feel tired but mentally alert when they get into bed.
Choosing the Right Device for Your Sleep Struggles

In practice, the best starting point is usually figuring out what is actually keeping you awake. If your sleep is being disrupted by noise, light, or an inconsistent routine, environmental tools are often enough to make a noticeable difference. If the main issue is stress or difficulty unwinding, then approaches that focus on calming the nervous system tend to be more helpful. And if those areas are reasonably well managed but you still struggle to fall asleep, a brain-focused approach may be more relevant.
In many cases, it is not about choosing one tool over another. Combining approaches can be more effective, especially when different factors are overlapping. For example, improving circadian rhythm with consistent light exposure while also addressing stress or pre-sleep alertness can create a more meaningful shift than either alone.
It’s also important to keep expectations realistic. Device-based sleep support works differently from medication. Instead of producing an immediate sedative effect, most of these tools work gradually by supporting the systems that regulate sleep. That can make progress feel slower at first, but often more sustainable when the approach matches the underlying issue.
Sleep improvement is rarely linear. Stress, routine, health, and environment all interact, so it is normal for results to vary night to night. These tools tend to work best when used consistently as part of a broader sleep strategy, rather than as standalone fixes.
Danielle (Dani) Mathieu is a health and medical writer who works with global health and wellbeing businesses to deliver insight-driven, research-backed content at the intersection of psychology and nursing. She has 18+ years of experience in communications, holds an MA in Psychology, and is currently studying for an MSc in Adult Nursing.
Dani is happiest when she’s translating complex health and nutrition science into plain-English stories that feel genuinely useful without being overwhelming. When she’s not juggling clinical placements on the ward, she’s usually writing. She lives on the Scottish coast, loves a cold sea breeze, and is often accompanied by a very opinionated dog.







